Question 5 of 5
(demo test)
Product Demo for BASIC Exam
-
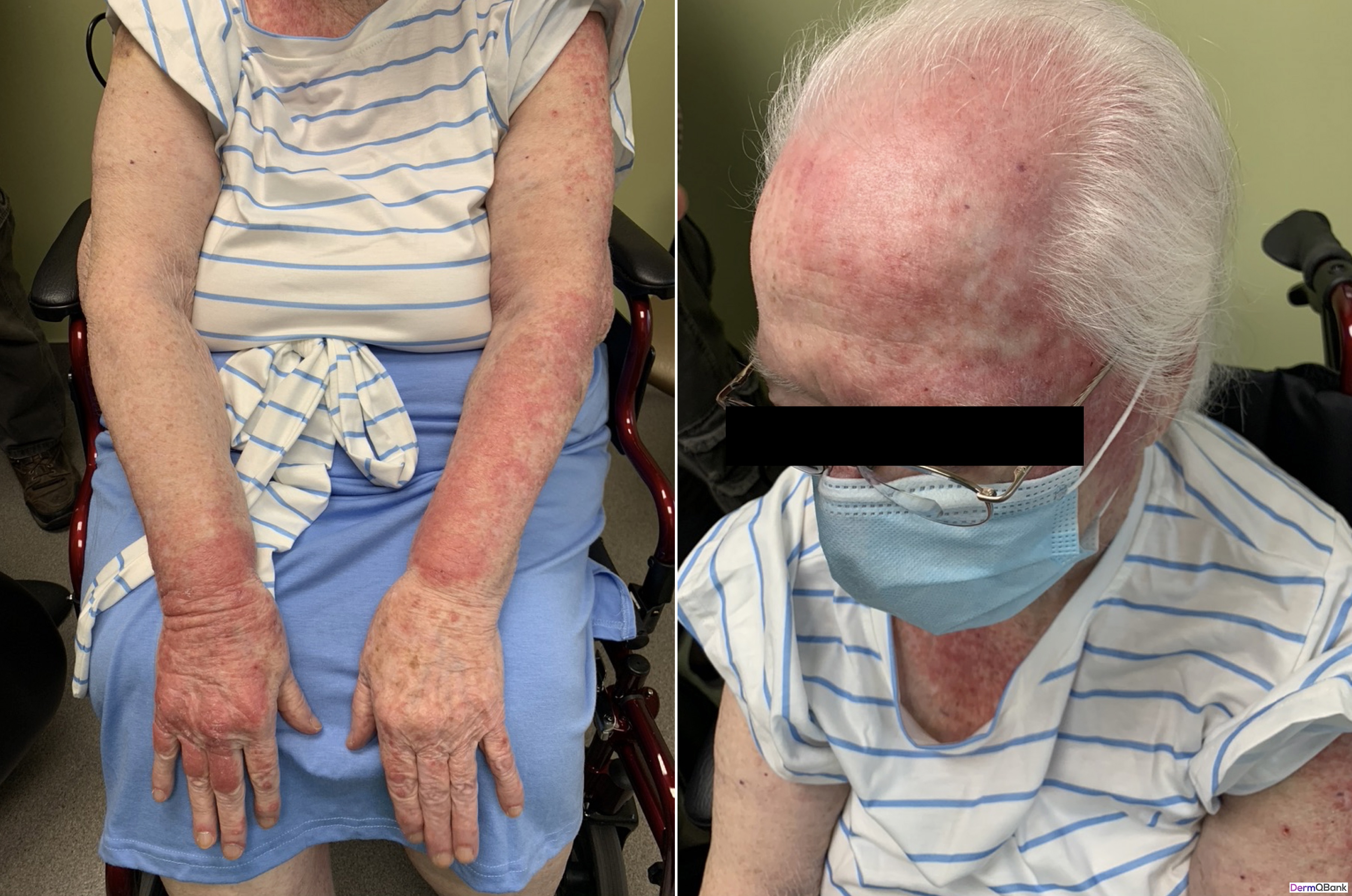
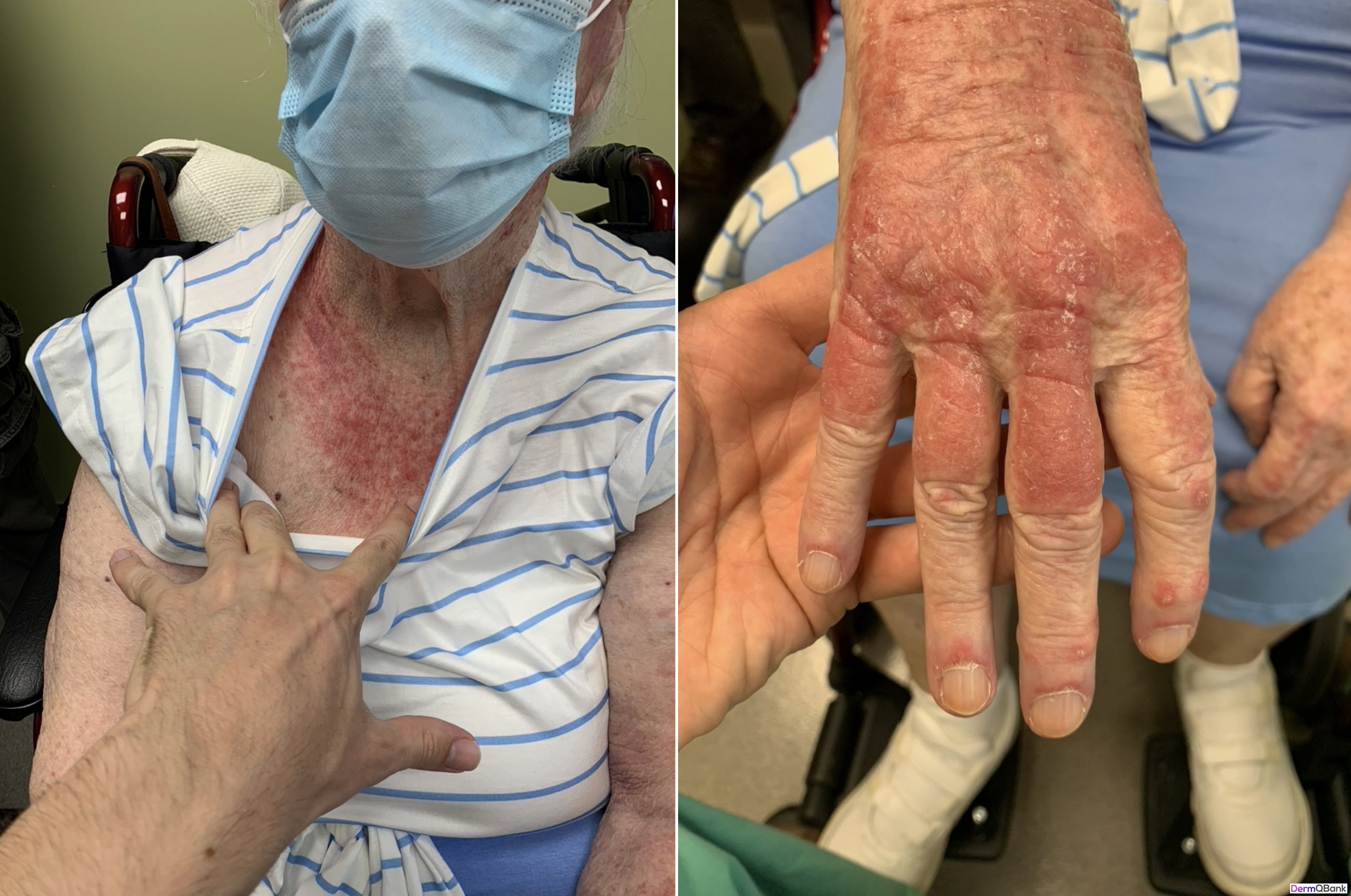
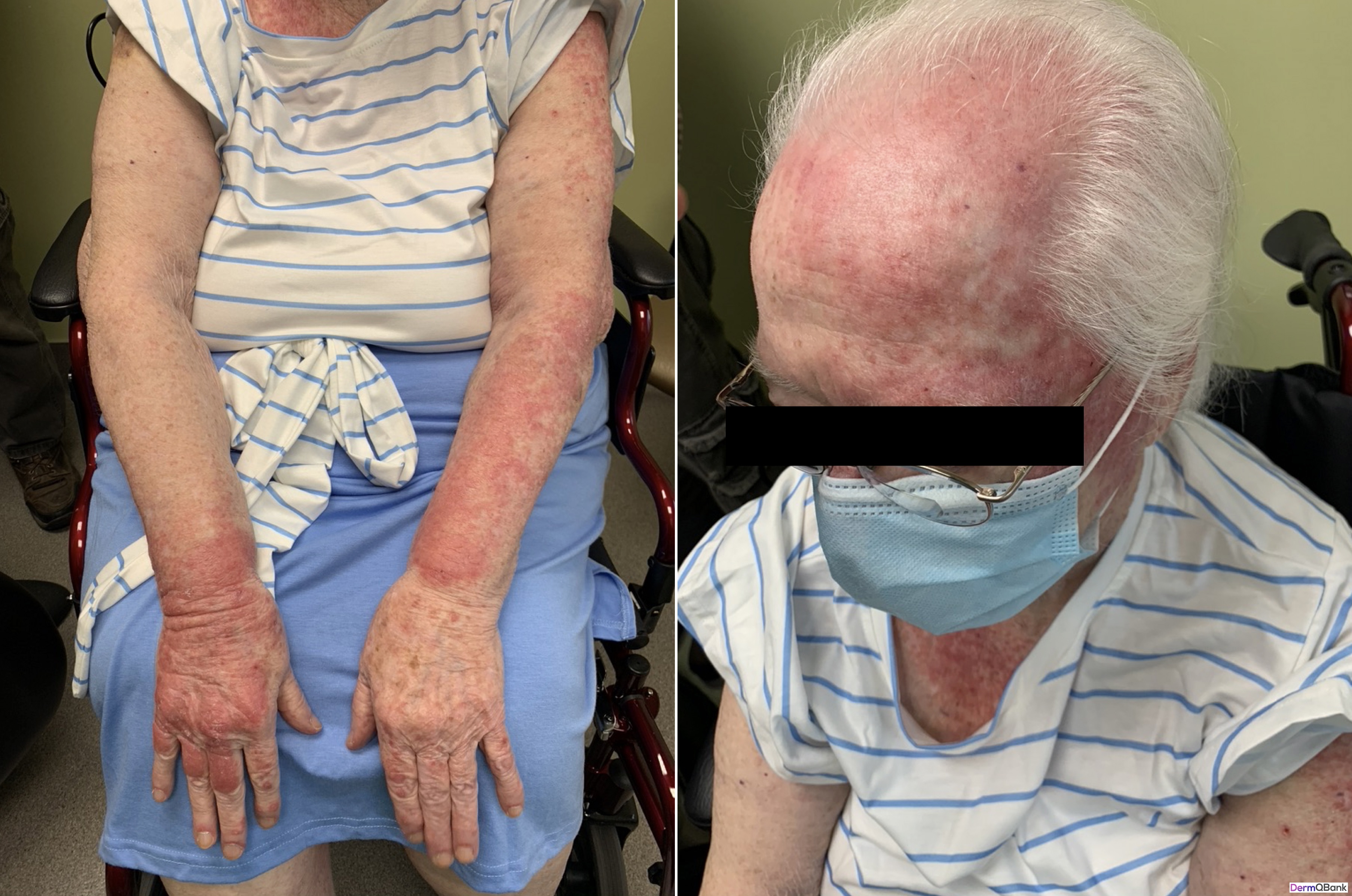
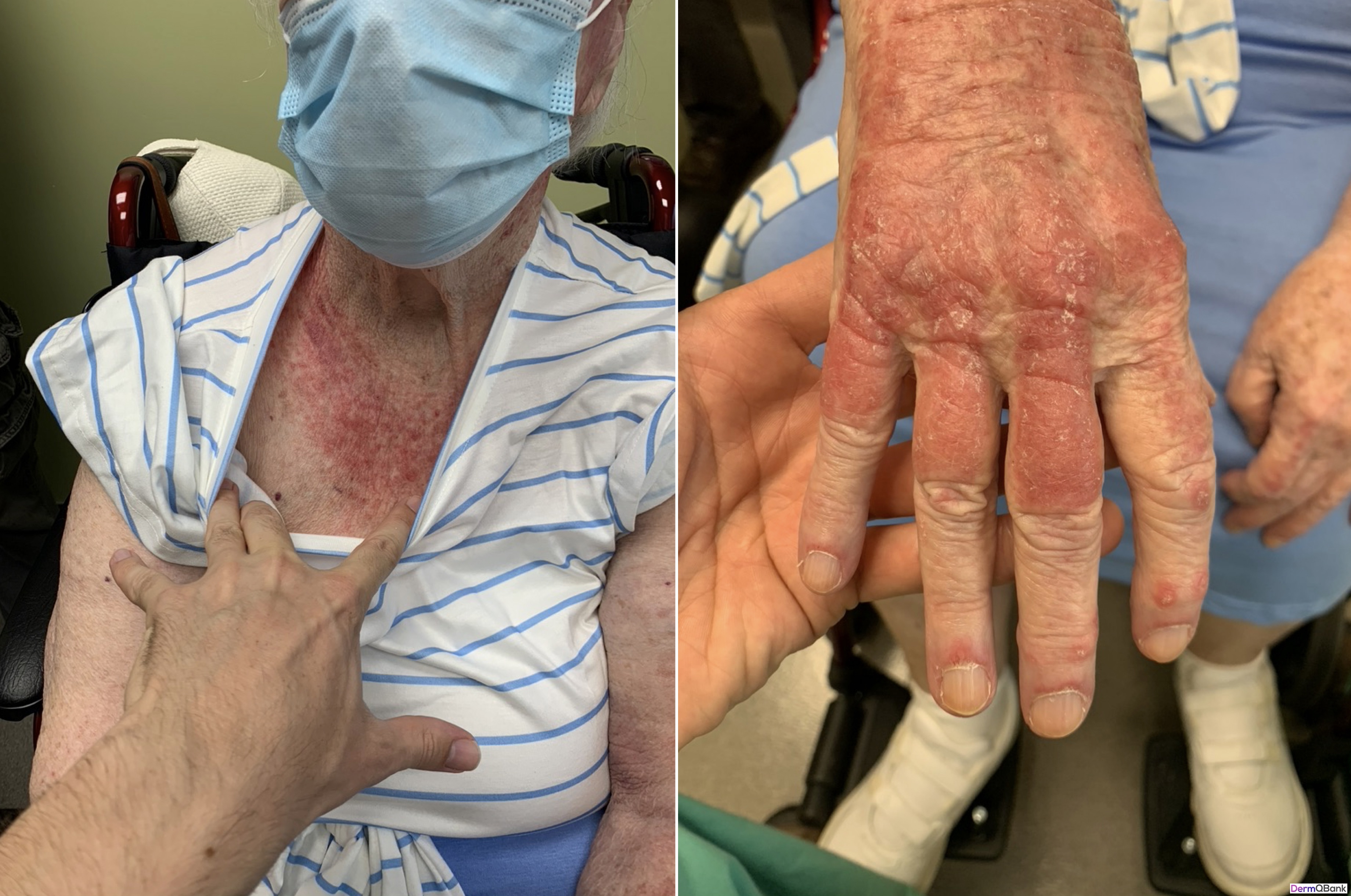
Which of the following is the most likely diagnosis?
This patient has classic dermatologic findings for dermatomyositis (DM).
DM is an inflammatory disorder which generally presents with characteristic skin findings and progressive muscle weakness. Early in training it can be difficult to distinguish DM from other photosensitive eruptions, particularly systemic lupus erythematosus (SLE) both clinically and histologically. A couple of helpful clinical clues that favor DM over SLE are the marked pruritus, the malar erythema that does not spare the nasolabial folds, and rash overlying the knuckles (rather than sparing the knuckles).
The nail fold changes seen in DM differ slightly from other diseases with nail fold changes including SLE and systemic sclerosis (SS). The poikiloderma seen in DM also differs slightly from the poikiloderma seen in SLE. These differences take practice to recognize. See CORE and APPLIED QBank for further detail.
The muscle disease associated with DM can also be difficult to distinguish from other idiopathic inflammatory myopathies (polymyositis and inclusion body myositis) and other connective tissue diseases.
Below is a thorough review of dermatomyositis testable factoids:
-
Clinical Features
- Can present in children and adults (bimodal) and is more common in women. Pediatric patients typically present between ages 5- and 15-years-old and adults are generally in their late 40's to early 60's
-
Dermatologic findings include:
- Distinctive photodistributed violaceous poikiloderma (hyperpigmentation, hypopigmentation, telangiectasias, epidermal atrophy) favoring the scalp, upper chest/back/shoulders (shawl sign), around the neck (V sign), extensor surfaces, and periocular region (heliotrope rash). Involvement of the hips is infrequent and referred to has the holster sign
- Dilatation and dropout of nail fold telangiectasias and ragged cuticles
- Gottron’s papules overlying knuckles (purple or red, occasionally scaly slightly raised papules that occur on any of the metacarpophalangeal joints or the interphalangeal joints of the fingers)
- Malar erythema which does not spare the nasolabial folds (this is in contrast to systemic lupus)
- Mechanic's hands (rough fissured skin of the tips and lateral surfaces of the digits resembling those of a manual laborer
- Raynaud's syndrome
- Anti-MDA5 DM and Wong-type DM are variants of DM with differing clinical features. Anti-MDA5 DM features are outlined below. Wong-type DM is a rare variant with cutaneous findings of keratotic follicular papules resembling pityriasis rubra pilaris (PRP) (See CORE and APPLIED Bank for further detail)
-
Non-dermatologic findings include:
- Progressive symmetric muscle weakness in the proximal muscles (e.g., shoulders and quadriceps) with associated laboratory signs of inflammatory myopathy
-
Diagnosis
- Skin histology shows an interface dermatitis plus mucin deposition
- Muscle biopsy shows lymphocytic myositis in affected muscles
- In diagnosing DM, a muscle biopsy of the triceps is preferred to the deltoid as the deltoid often does not become involved until later in the disease
- Recognizing clinical features and confirming with biopsies (skin and/or muscle), imaging (MRI or ultrasound), and laboratory evaluation, can lead to early diagnosis and appropriate treatment including appropriate malignancy screening and detection of interstitial lung disease or other internal organ involvement
- Ultrasound and/or MRI of the proximal muscles may be obtained instead of triceps muscle biopsy and are sensitive tests in the diagnosis of DM. MRI is the most sensitive test for diagnosing DM-associated myositis, however, ultrasound is a cheap option, particularly for those with classic disease. MRI may also help to differentiate between dermatomyositis and polymyositis
-
High-yield DM antibody associations
- ANA: positive in ~70% of patients. Present in nearly all patients with SLE and therefore of little utility in differentiating DM and SLE
- Antisynthetase antibodies (anti-Jo-1, anti-PL-7, and anti-PL-12): linked to a high risk of interstitial lung disease
- Anti-SRP: linked to acute-onset necrotizing myopathy with severe weakness and high serum creatine kinase
- Anti-p155/140: linked to higher risk of cancer
- Anti-p140 (anti-NXP2): linked to juvenile DM with calcinosis as well as increased risk of malignancy
- Anti-SAE: linked to adult dermatomyositis and amyopathic dermatomyositis
- Anti-Mi-2: linked to cutaneous findings (shawl sign, cuticular changes) and milder muscle disease with good prognosis. The most specific antibody for dermatomyositis
- Anti-CADM-140/MDA5: linked to amyopathic dermatomyositis and rapidly progressive interstitial lung disease that can be fatal. Also seen in a subset of patients with dermatomyositis with clinical features that differ substantially from classic adult DM (cutaneous/oral ulcers, painful palmar papules, alopecia, arthritis, panniculitis, and lower risk of myositis)
-
Management
- Management of cutaneous disease is via skin-directed therapy
- Management of myositis includes systemic corticosteroids and steroid-sparing immunosuppressant
- In adults, malignancy screening should be performed annually (and sooner if symptoms are present) for at least 3 years following diagnosis. The malignancy risk likely returns to baseline after 2-5 years
- While ~25% of adult dermatomyositis patients have an occult malignancy, there is no increased risk of malignancy in juvenile DM. Thus, children do not need to be evaluated for underlying malignancy when patients do not have symptoms that would suggest malignancy
-
Differential diagnosis
-
Includes other diseases with poikiloderma, photosensitive eruptions, disorders with favoring extensors
- SLE (photosensitive, poikilodermatous, nailfold telangiectasias)
- Psoriasis (favoring extensors)
- Photodrug (photodistributed)
- Cutaneous T-cell lymphoma (poikilodermatous)
- Allergic contact dermatitis (pruritic and eyelid edema similar to eyelid dermatitis)
- Scleroderma (nailfold telangiectasias)
- Other connective tissue diseases (overlapping clinical findings and antibody profiles)
-
Includes other diseases with poikiloderma, photosensitive eruptions, disorders with favoring extensors
Clinical Pearl: Dermatomyositis is an idiopathic inflammatory myopathy with symmetric proximal extensor muscle weakness and characteristic skin findings. Clinically, it can be difficult to distinguish from other idiopathic inflammatory myopathies (polymyositis and inclusion body myositis) and other connective tissue diseases including SLE. Recognizing clinical features and confirming with biopsies (skin and/or muscle), imaging (MRI or US), and laboratory evaluation including detection of certain antibodies, can lead to early diagnosis and appropriate treatment including appropriate malignancy screening and detection if interstitial lung disease, or other internal organ involvement.
References:
(