Question 1 of 5
(demo test)
Product Demo for BASIC Exam
-
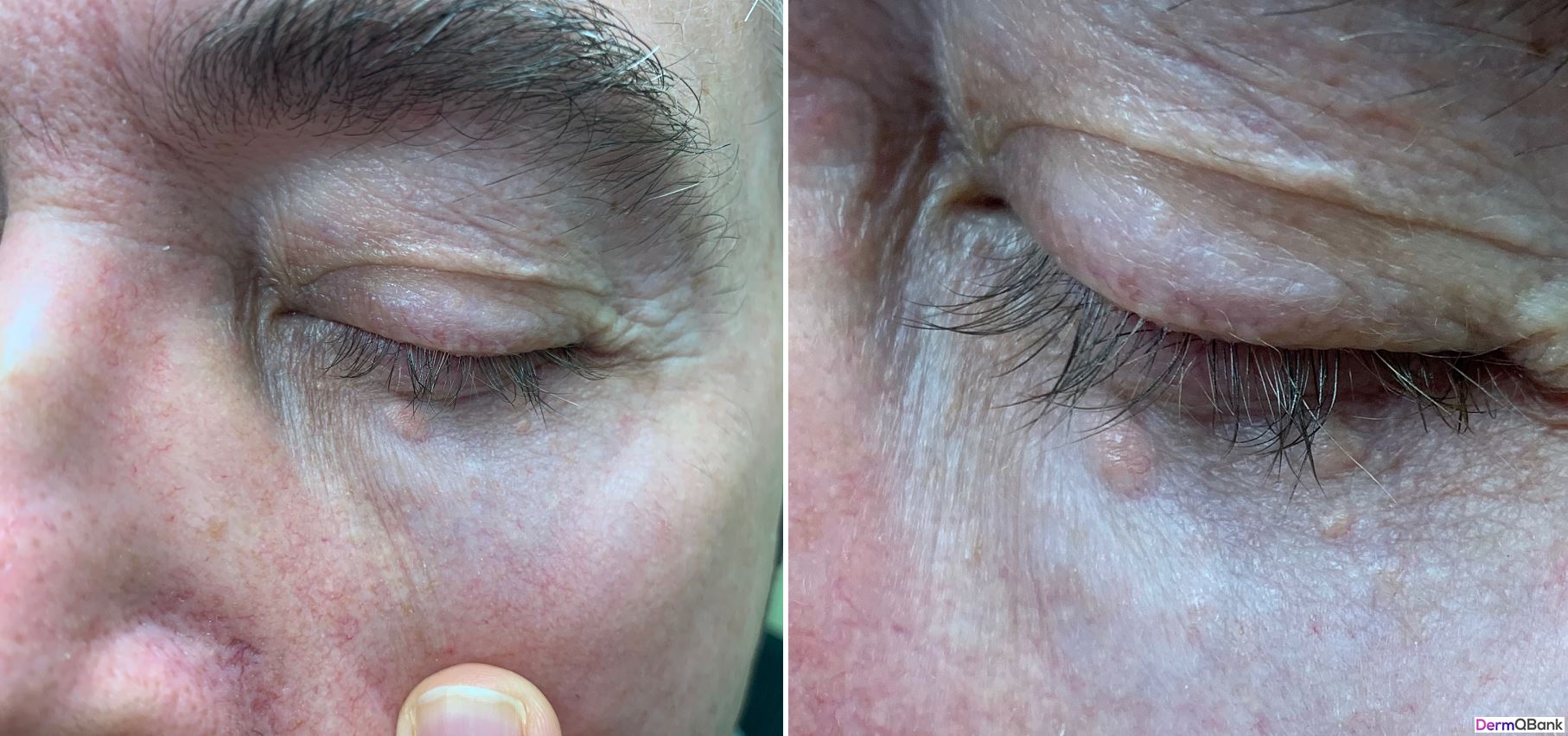
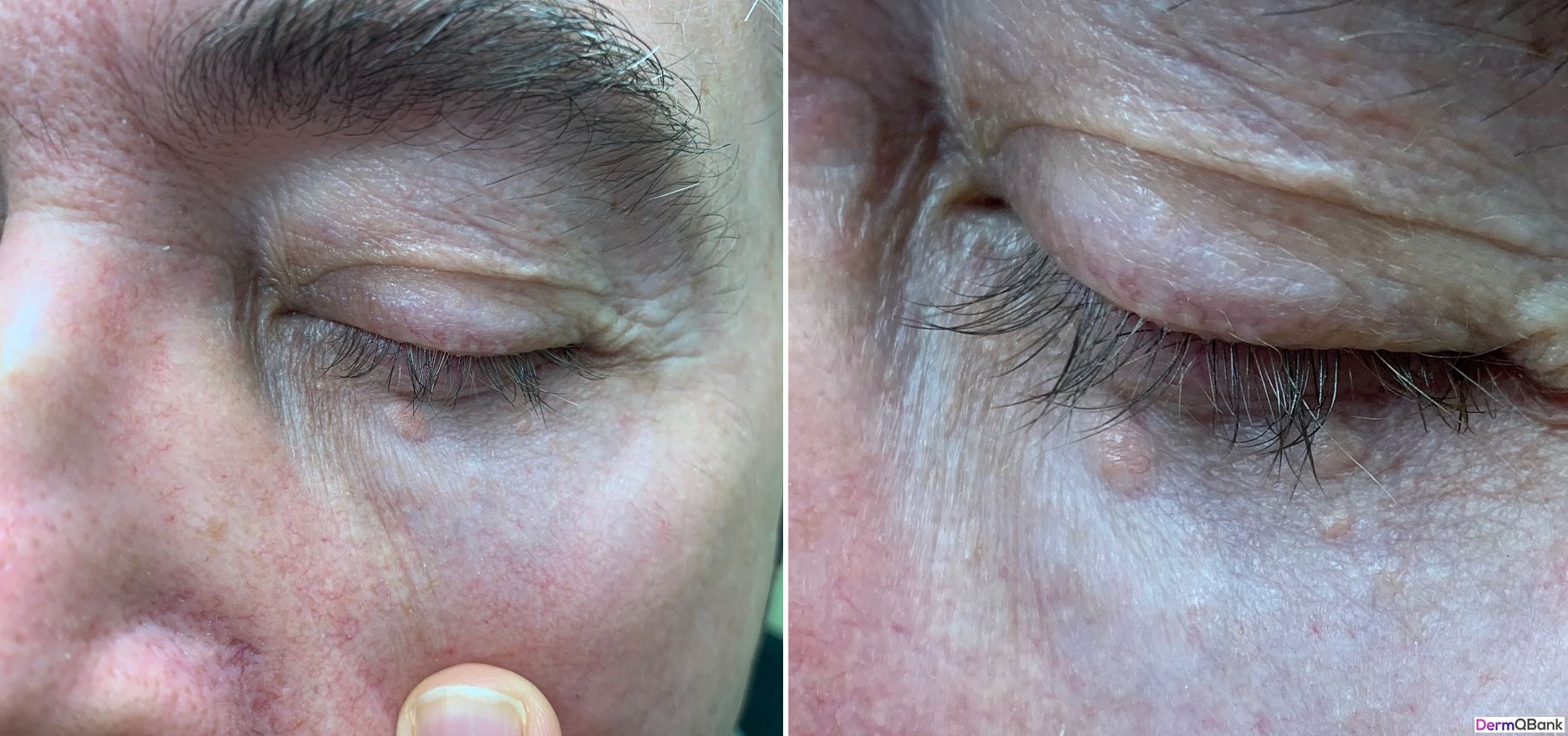
The pictured patient presents to clinic with a chief complaint of a bothersome lesion involving the left lower eyelid. A biopsy is performed. Clinicopathological correlation is most consistent with which of the following entities?
Dermatopathology
Common Disorders and Histologic Presentations
U
A
This is a benign syringoma. Take note of the multiple other similar but smaller lesions in the clinical photo. Similar to many other dermatologic disorders, clinical correlation may be necessary to confirm the appropriate dermatopathology diagnosis.
The dermatopathology differential diagnosis for a syringoma includes several more concerning lesions including sclerosing basal cell carcinoma, microcytic adnexal carcinoma, desmoplastic trichoepithelioma, and metastatic adenocarcinoma, therefore in the case of this biopsied syringoma, clinicopathological correlation, repeat biopsy, and/or a deeper punch biopsy may be required to rule out these other diagnoses. In this case, the clinical picture was clear and therefore no further testing was required.
As an experienced dermatologist, you will learn to anticipate histologic findings based on lesion morphology and other clinical findings. The same is true for an experienced dermatopathologist, who can narrow down their histologic diagnosis based on clinical data provided by the dermatologist.
Below is a brief review of syringomas:
- Benign adnexal neoplasm with mostly ductal differentiation (syringeal differentiation)
- Can be used to describe lesions of either apocrine or eccrine lineage
- Common clinical lesions presenting as multiple clustered small, firm, skin-colored smooth papules favoring the periorbital and eyelid skin. They can occur anywhere including the upper ventral trunk or genital skin
- Eruptive syringomas favor the trunk but can also occur on the palms and soles
- Syringoma-like changes can also be seen in cicatricial and non-cicatricial alopecias
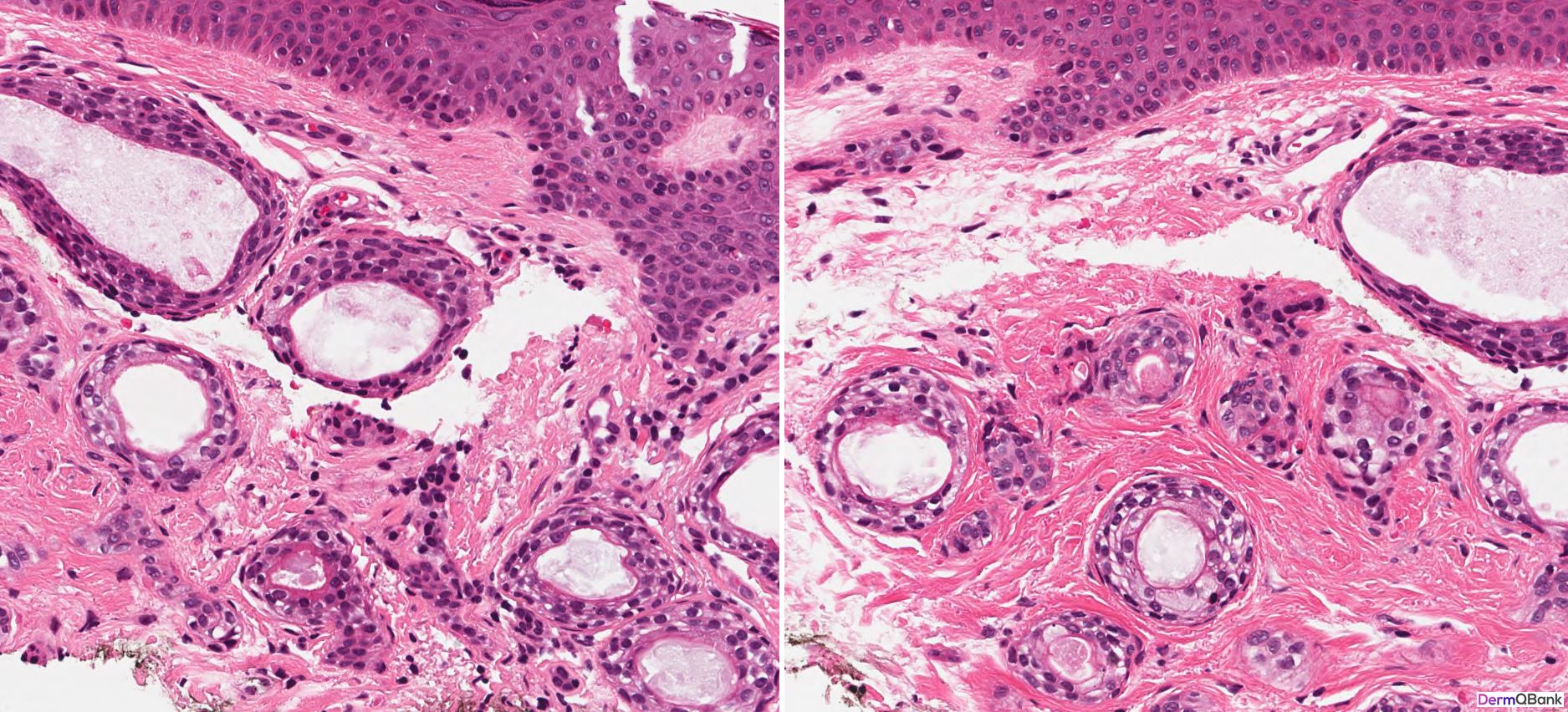
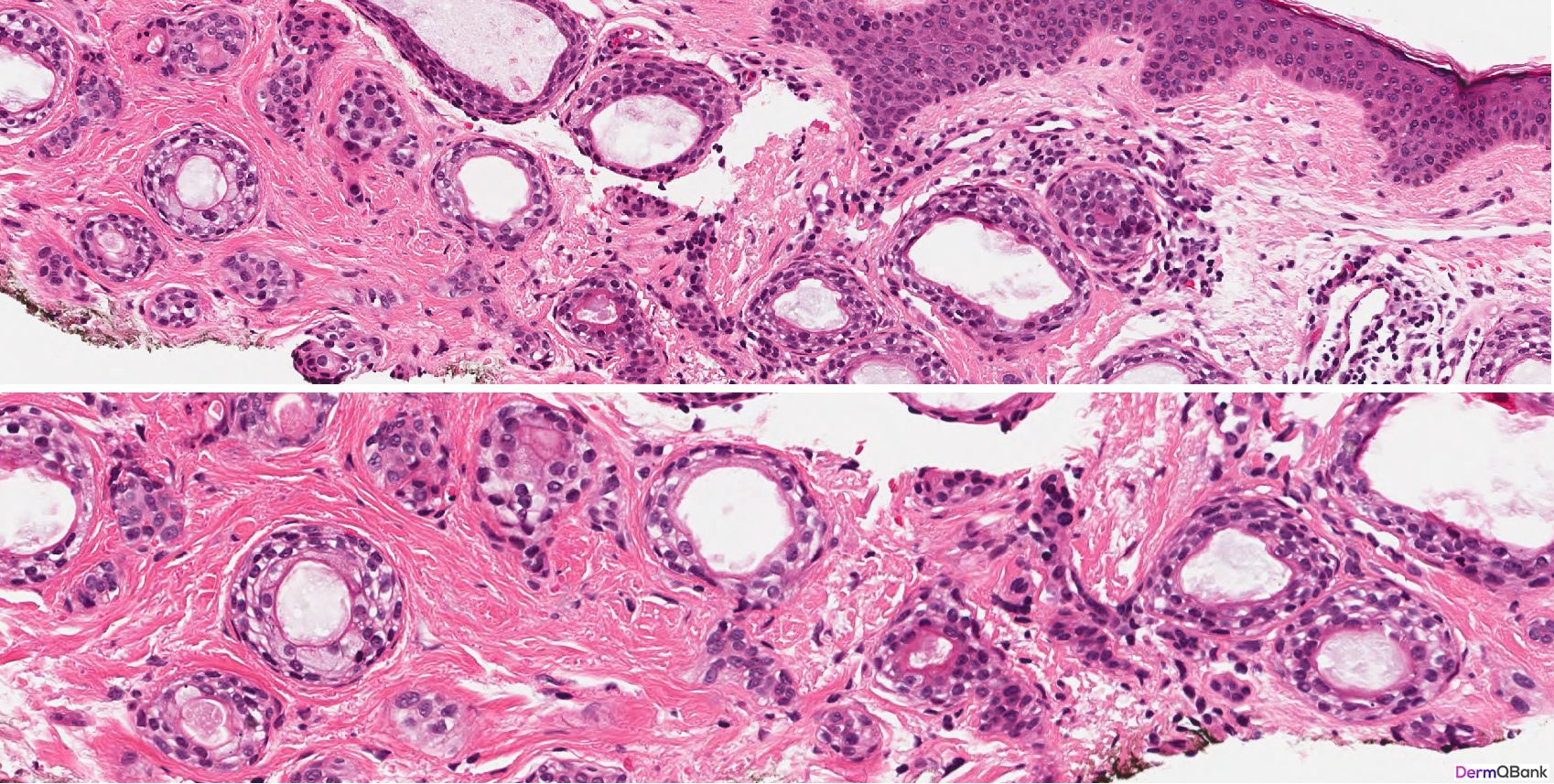
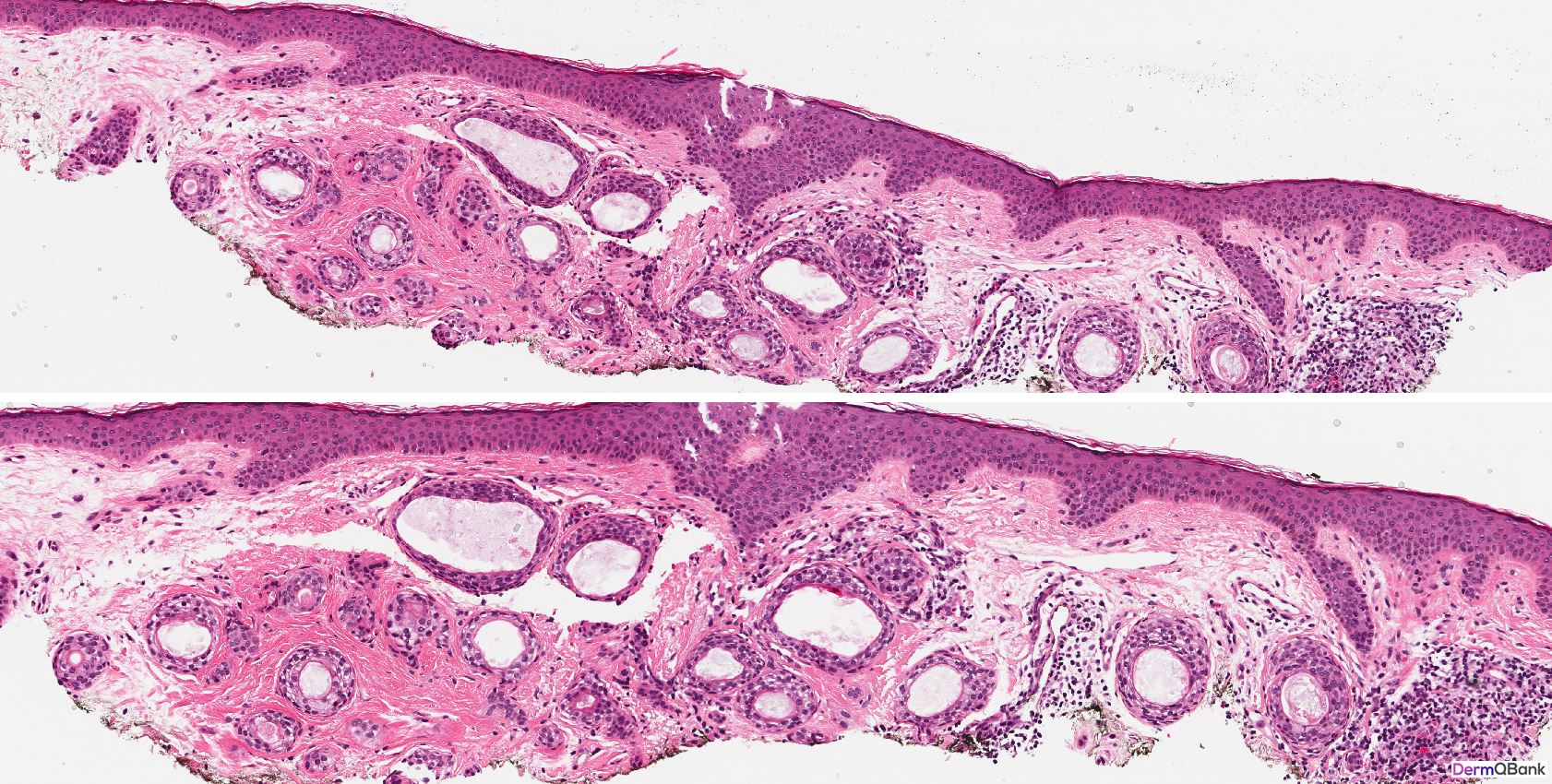
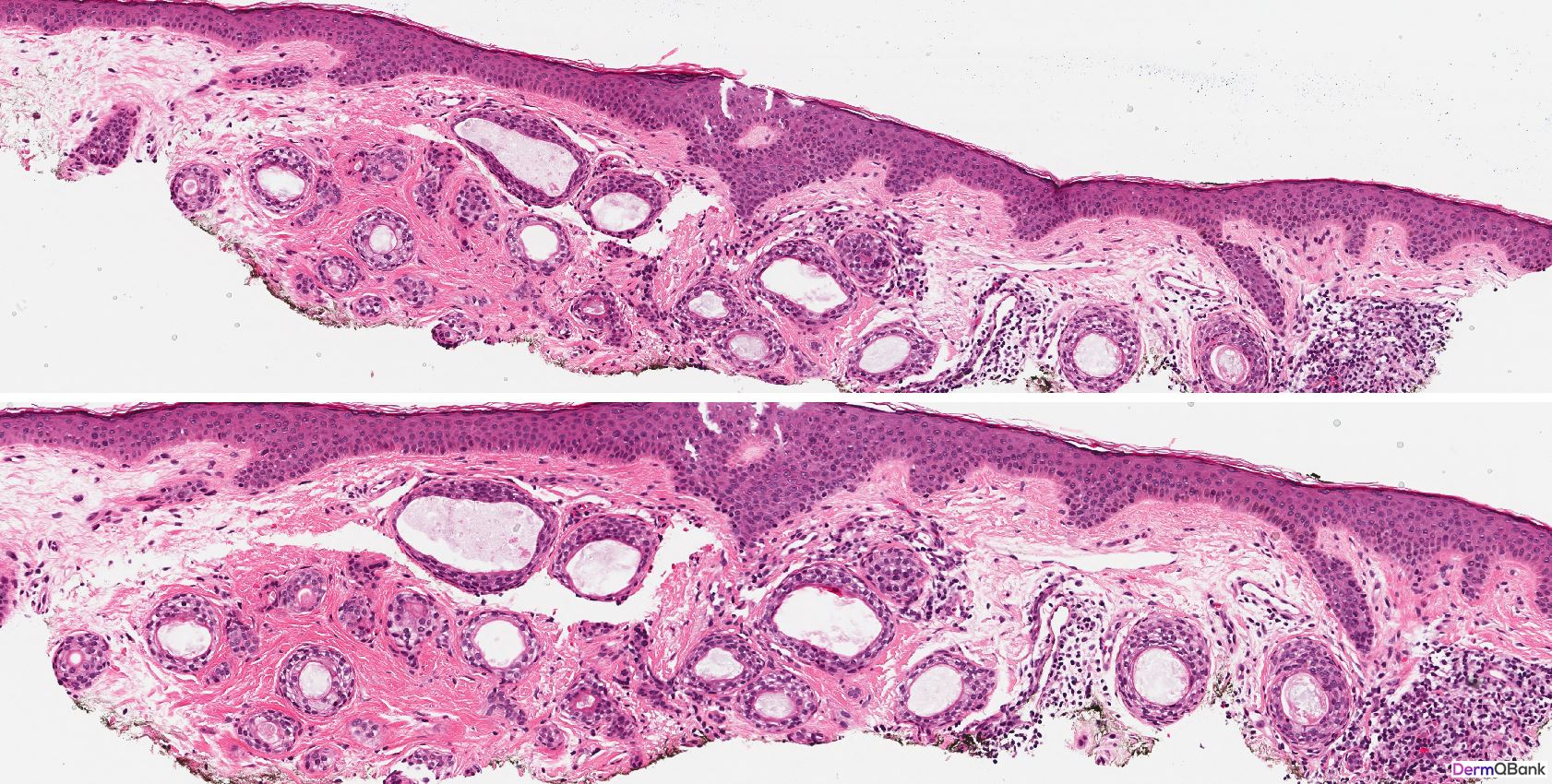
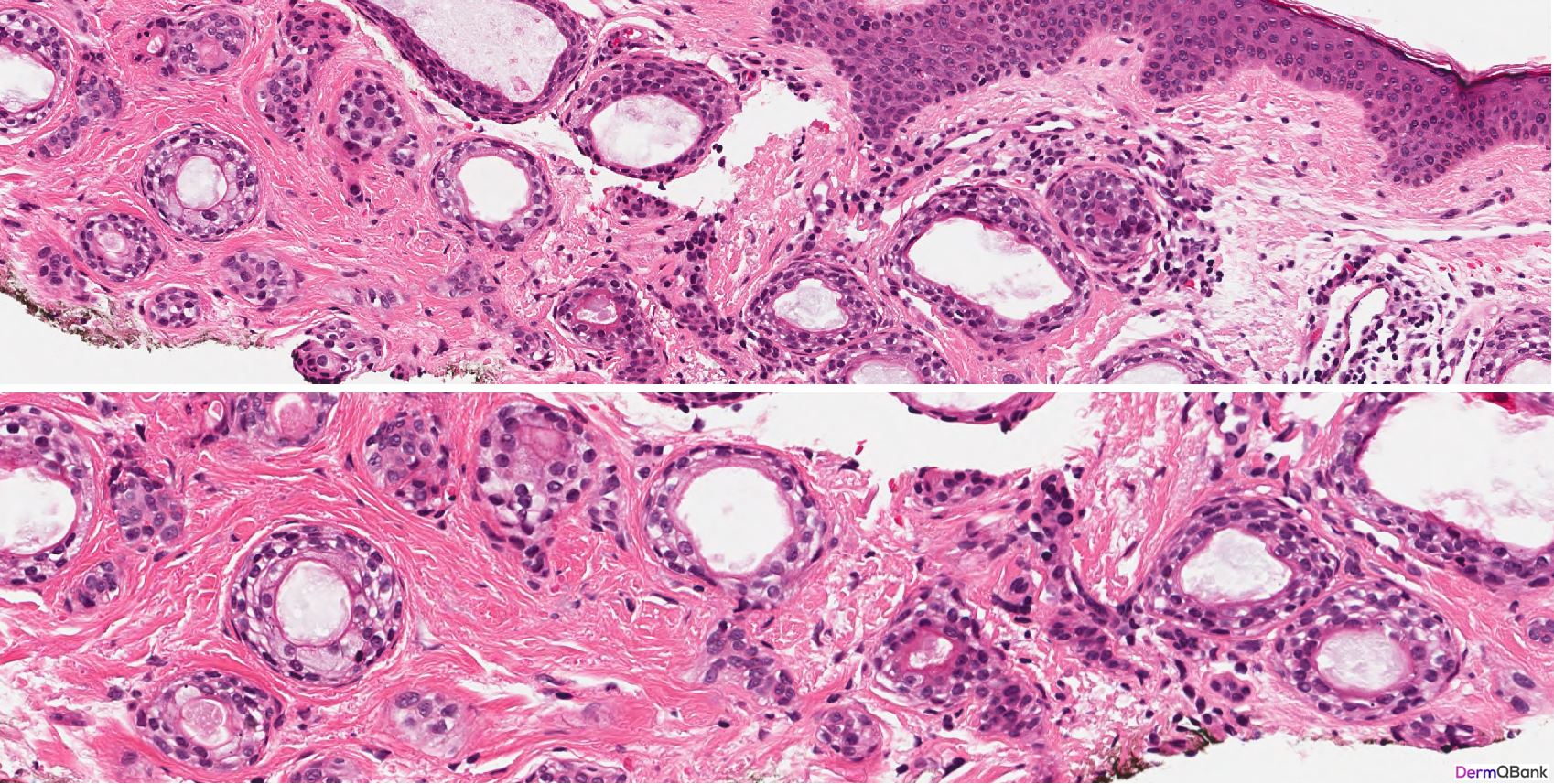
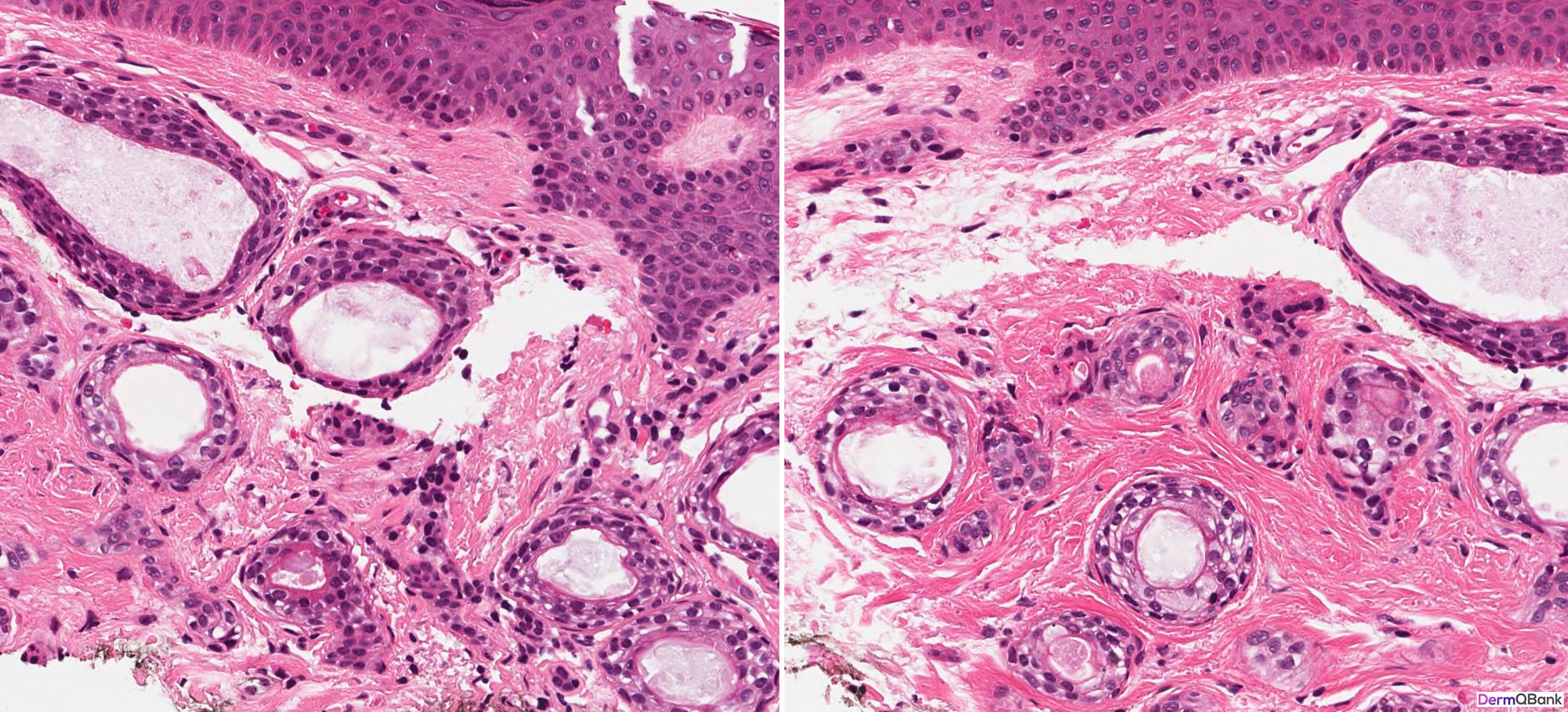
- Histology shows a circumscribed superficial proliferation of cells with a pale or pinkish cytoplasm forming nests and tubules relatively uniform in size within a sclerotic stroma. Dependent on the plane of sectioning, the nests of a syringoma vary in shape and some may assume a comma or tadpole shape. Tubular areas show ductal differentiation with a central lumina lined by a compact eosinophilic cuticle. Horn cysts and milia can also be observed
- Usually not associated with any underlying abnormality, however, multiple lesions can be associated with systemic syndromes; Down syndrome being the most common. (Williams et al. J Am Acad Dermatol 2016)
The histologic differential diagnosis of syringomas includes the following:
- Desmoplastic trichoepithelioma
- Microcystic adnexal carcinoma
- Sclerosing basal cell carcinoma
- Metastatic adenocarcinoma
Microcystic adnexal carcinoma (MAC) is a low-grade adnexal carcinoma also know as sclerosing sweat duct carcinoma. It is most commonly encountered on the nose and upper cutaneous lip in young adult women and is likely related to UV exposure. A typical clinical presentation is as a slowly enlarging sclerotic indurated appearing pearly papule or plaque on the face of a young or middle-aged adult. (Chiller et al. Arch Dermatol 2000) Histopathology reveals asymmetric, infiltrative basaloid strands with small lumina, and sweat gland and/or follicular differentiation in a hyalinized stroma. Perineural invasion is often seen as is solar elastosis and horn cysts.
Morpheaform basal cell carcinomas is a less common subtype of basal cell carcinoma that may clinically resemble a scar. Lesions can be slightly elevated or depressed with an area of white or light pink induration. Dermoscopy is a helpful tool when the diagnosis is in question. Histopathology shows thin strands or cords of invasive basaloid cells in a fibrotic stroma. The peripheral palisading and stromal retraction that is seen in other subtypes of basal cell carcinoma are typically absent. Lesions tend to have a higher degree of atypia, mitoses, and apoptotic bodies compared to MAC. Perineural invasion (PNI) is rarely seen.
Desmoplastic trichoepitheliomas typically present as a solitary firm skin-colored to pink annular plaque with a central dell. The typical presentation is small isolated lesion on the cheek of a woman. Histopathology shows a circumscribed lesion composed of cords of basaloid cells ~2 cells thick winding through thick collagen bundles in the upper 2/3 of the dermis. Cytologically bland keratocysts may be present. It can be very difficult to differentiate a desmoplastic trichoepithelioma from MAC with a superficial biopsy. However, MACs are much more infiltrative and PNI is characteristic and not seen in desmoplastic trichoepithelioma. If ductal differentiation is seen, desmoplastic trichoepthelioma can be excluded.
Clinical Pearl: Syringomas are common clinical lesions presenting as multiple clustered small, firm, skin-colored smooth papules favoring the periorbital and eyelid skin. As the histologic differential diagnosis includes several more concerning lesions, be able to recognize the histology findings in a syringoma and differentiate these findings from common mimickers. A syringoma is a circumscribed proliferation of eccrine-like ducts in the superficial dermis within a fibrotic stroma resembling "tadpoles" swimming in the superficial dermis.
Other References:
(Busam, Klaus. Dermatopathology: Foundations in Diagnostic Pathology. Saunders Elsevier. 2010)
Heads up! You can use keyboard for test navigation: press → for Next,
← for Previous, M for Mark/Unmark, P for Pause,
R for Review, A,B,C,... or 1,2,3,... to select answer.